Protective effect of Vitamin D on Cardiac Mitochondrial Apoptotic pathway in Rats fed with high fat diet
Received: March 25, 2019
Accepted: April 03, 2019
Published: May 05, 2019
Genet.Mol.Res. 19(5):
Keywords
Apoptosis; Heart; Vitamin D; High fat diet.
Introduction
Obesity is becoming a global epidemic in both children and adult (World Health Organization, 2015). It described as an extreme quantity of body fat or adipose tissues in relative to slim body build (World Health Organization, 2015). It is related with many diseases such as heart and circulatory disorder, metabolic syndrome, increase blood pressure, stroke and coronary artery disease (Fitchett D, 2015; Chorin E, Hassidim A, Hartal M, Havakuk O, et al., 2015). Obesity may affect the heart through its influence on known risk factors such as dyslipidemias, hypertension, glucose intolerance, and inflammatory markers (Hubert HB, Feinleib M, McNamara PM, Castelli WP, 1983), these abnormalities could relate to genetic alterations (Swinburn B and Egger G, 2002). Reports account a persistent rise in the incidence of obesity in the previous 3 years in Saudi Arabia. From previous 1980 till middle-1990, general incidence of obesity was predictable by twenty percent (Kang JH and Kang JY 2015; Dyson J, Jaques B, Chattopadyhay D, Lochan R; 2014).
Memish et al. proved that the deteriorating tendency in incidence of increase in weight alarmed the young adult, in contrast among the old adult where the tendency was increase. Irrespective this repartition, the important reduction of fatness in our kingdom is a suitable reveal of the efficiency of native healthiness trials and strategy to regulator the obesity, and the responsiveness operations assumed by the Saudi ministry of health, over the previous period, which concentrated on behavioral and dietary alterations (Memish ZA, Bcheraoui C, Tuffaha M, Robinson M, 2014). An increase in the body mass index more than thirty was observed to be related with vitamin D deficiency. Several studies and clinical analyses have exposed a close association with vitamin D deficiency and heart circulatory system disorder (Earthman CP, Beekman LM, Masodkarand K, Siblay SD, 2012). Deficiency of Vitamin D has been indicated to be extremely widespread among wide-ranging population with several chronic illnesses involving heart and circulatory disorder which may be a prominent cause of death (Assalin HA, Rafacho B, Santos P, Ardisson L, 2013).
While Saudi Arabia has sunshine weather throughout the year, the population do not display themselves to daylight as reported by Ardawi et al. (2012). Numerous reports revealed that a vitamin D deficiency give rise to cardiac alterations. Yet, the underline mechanism need to be further clarified. The impact of the extent of VD deficient on cardiac muscle is undetermined.
Method
Wistar rats (male) weighing in the range of 150-200 g were housed in standard laboratory conditions with temperature of 23 ± 3°C and a natural light conditions with 12 hours light/dark cycle along with free access to water ad libitum. In accordance with the guidelines approved by the institutional ethical committee, all the rats were reared under the laboratory conditions that avoided them from experiencing unnecessary pain and discomfort. The experimental rats were randomly grouped/assigned to receive either the standard diet (D12450H), which are regarded as normal control rats or high-fat diet (D12451) considered as high-fat diet group of rats. Diet composition is detailed in Table 1.
| (DIO) Formulas(12) | D12451 Match 17% Sucrose(12) | |||
|---|---|---|---|---|
| Product # | D12451 | D12450H | ||
| gm% | kcal% | gm% | kcal% | |
| Protein | 24 | 20 | 19.2 | 20.0 |
| Carbohydrate | 41 | 35 | 67.3 | 70.0 |
| Fat | 24 | 45 | 4.3 | 10.0 |
| Total | 100 | 100.0 | ||
| kcal/gm | 4.73 | 3.85 | ||
| Ingredient | gm | Kcal | gm | Kcal |
| Casein, 30 Mesh | 200 | 800 | 200 | 800 |
| L-Cystine | 3 | 12 | 3 | 12 |
| Corn Starch | 72.8 | 291 | 452.2 | 1808.8 |
| Maltodextrin 10 | 100 | 400 | 75 | 300 |
| Sucrose | 172.8 | 691 | 172.8 | 800 |
| Cellulose, BW200 | 50 | 0 | 50 | 0 |
| Soybean Oil | 25 | 225 | 25 | 225 |
| Lard | 177.5 | 1598 | 20 | 180 |
| Mineral Mix S10026 | 10 | 0 | 10 | 0 |
| DiCalcium Phosphate | 13 | 0 | 13 | 0 |
| Calcium Carbonate | 5.5 | 0 | 5.5 | 0 |
| Potassium Citrate, 1 H2O | 16.5 | 0 | 16.5 | 0 |
| Vitamin Mix V10001 | 10 | 40 | 10 | 40 |
| Choline Bitartrate | 2 | 0 | 2 | 0 |
| FD&C Red Dye #40 | 0.05 | 0 | 0.04 | 0 |
| FD&C Blue Dye #1 | 0.01 | 0 | ||
| Total | 858.15 | 4057 | 1055.05 | 4057 |
Table 1: DIO series diets (research diet center).
Experimental Protocol
25 wistar rats were included in current study and randomly distributed into the following groups:
• Control group (C): rats received the standard diet (n=5 rats).
• High fat diet fed group (HFD): The group of rats were fed with a high fat diet (HFD) for a total of six months (n=10 rats)
• High fat diet fed group + vitamin D group (HFD+VD): The group of rats fed with a high fat diet (HFD) daily with oral gavage supplemented with vitamin D at the rate of 400 IU/kg (n=10 rats).
Vitamin D was given by means of gavaging technique at a dose of 400 IU/kg/day (Vieth R, 2004). The study continued for sixth months, body weight and oral –anus (OA) length were measured every 45 days to assess body mass index (BMI). Towards the end of the experimental schedule, the experimental rats were sacrificed under the effect of diethyl ether and the heart specimens were kept in RNA later for Quantitative Real-time polymerase chain reaction (qRT-PCR based analysis).
RNA extraction
Following the manufacturer instructions and using the column purification technology by RNeasy Mini Kit (Qiagen), the total RNA was isolated from the cells.
Reverse transcription
Using cDNA reverse transcription kit (ImProm-II™ ReverseTranscription System cat no. A3800) and following the manufacturer procedure, the reverse transcription of the separated RNA into the complementary deoxyribonucleic acid (cDNA) was carried out.
Quantitative Real-Time Polymerase Chain Reaction (qRT-PCR)
The quantitative real-time polymerase chain reaction (qRT-PCR) was performed using the KAPA SYBR® FAST qPCR Kit Master Mix (2X) Universal with the Cat no. KR0389. The below mentioned rat primers were used for the PCR: rat Bcl2 forward primer AGTGGGATACTGGAGATG: rat Bcl2 reverse primer CTGGCTGTCTCTGAAGAC: rat BAX forward primer CTGGACAACAACATGGAGC: rat Bax reverse primer CAGACGGCAACTTCAACTG.
Statistical Analysis
The data obtained were subjected to statistical analysis of using SPSS for windows package version 23. (SPSS Inc., Chicago, IL, USA). The analysed data are reported in terms of mean ± SD for gene expression. In order to make comparison of the response, between the control and the experimental groups, one way analysis of variance (ANOVA) test was applied. The Rq values obtained for each gene was compared using one-tailed student’s t-test. The differences were considered statistically significant, if the p value was found to be either less than or equal to 0.05.
Results
The results obtained from the present study are presented in Table 2, and also illustrated in Figure 1, 2 and 3.
| Groups | Genes (Relative Expression) | |
|---|---|---|
| Bax | Bcl2 | |
| C | 0.278 ± 1.32 | 18.892 ± 1.73 |
| HFD | 220.494 ± 1.76 | 2.945 ± 0.30 |
| HFD +VD | 1.556 ± 0.92 | 5.093 ± 1.65 |
C: Control rats, HFD: Rats Fed With High Fat Diet, HFD +VD: rats fed with high fat diet treated with vitamin D. Values are expressed in the form of mean ± SEM.
Table 2: Comparative expression level of target genes in control and each of the experimental group in comparison to reference gene, RE = 2 [ΔCT] = 2 [CT reference gene –CT target gene]
1-Differences in the body weight, oral –anus (OA) length and the body mass index (BMI):
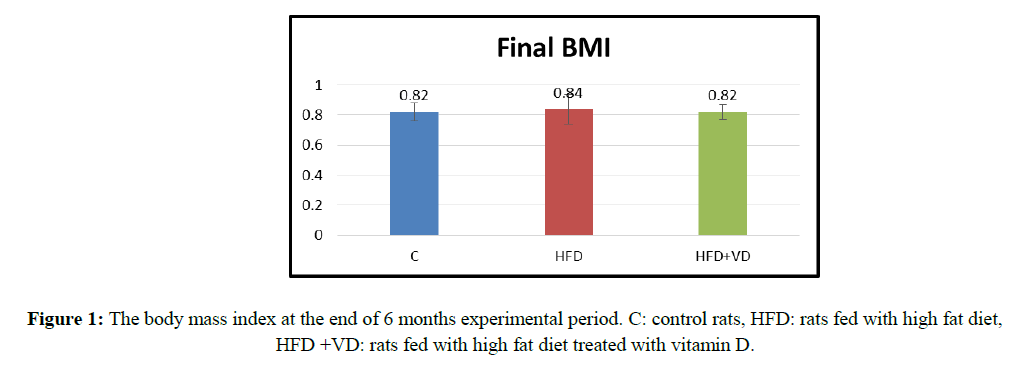
At the end of the experimental period of six months, the body weight, the length of the body (oral –anus (OA)), as well as the body mass index (BMI) were found not significantly different in the experimental group when compared to their respective controls (Figure 1).
2-Quantitative Real-time polymerase chain reaction (qRT-PCR):
BAX and BCL2 polypeptides
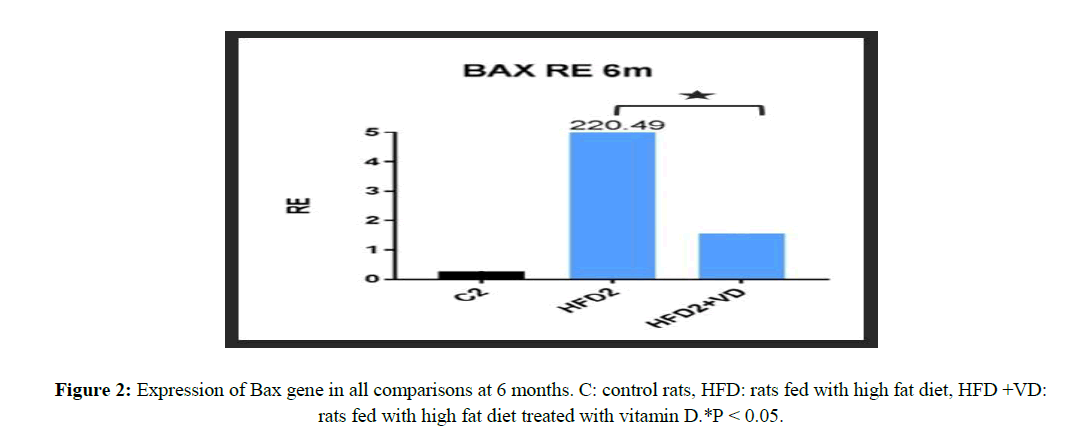
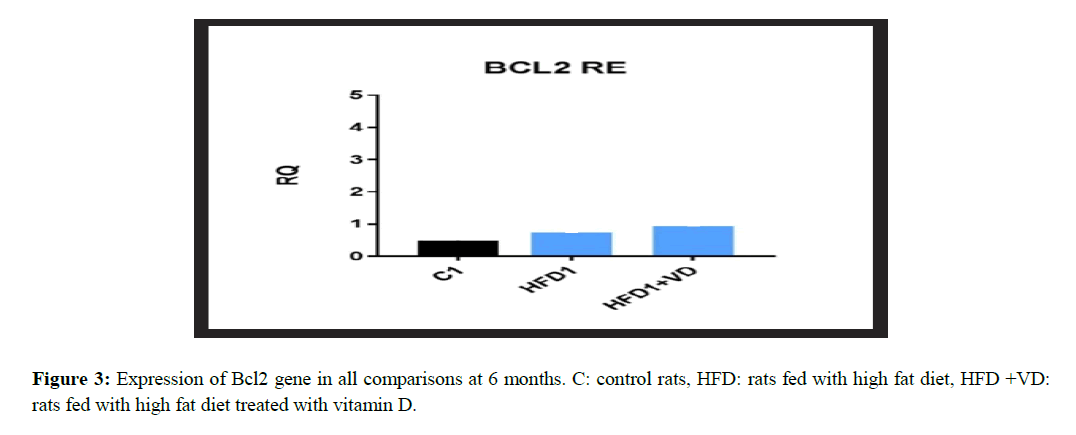
The mitochondrial-dependent apoptotic pathway was analyzed by means of measuring the expression level of the anti-apoptotic BCL2 and pro-apoptotic Bax proteins. At the end of experimental period of 6 months, BCL2 was found to be down-regulated while pro-apoptotic BAX was found to be significantly upregulated by high fat diet (HFD) consumption. Vitamin D supplementation with the high fat diet (HFD) increased BCL2 expression, although did not reach significance, while vitamin D significantly decreased Bax expression when compared to high fat diet group (Table 2, Figures 2 and 3).
Discussion
There has been a substantial increase in the prevalence of nutrition associated diseases, such as obesity, diabetes and cardiovascular diseases over the past few decades. The nutritional quality of the diet could be one of the most important factors/causes associated with hypertriglyceridemia, hyperglycemia, and hypertension, decreased level of high-density lipoprotein-cholesterol and even in the increased abdominal circumference (Ramalho et al., 2017). Previously studied were conducted with high fat diet (HFD) in experimental animals, particularly in mice and rats. Some of these animal studies have associated high fat diet (HFD) intake with hyperphagia, weight gain and increased adiposity (Woods SC et al., 2003), while other studies associated high fat diet (HFD) consumption to hyperinsulinemia, insulin resistance without developing obesity (Ramalho et al., 2017).
The present experimental study using laboratory animals was comprised of control group (fed with standard diet containing 10% fat), on experimental group of rats termed HFD-fed group (fed with diet containing 45% fat), and another experimental group of rats termed HFD-fed group (fed with HFD supplemented with vitamin D). At the end of the experiment of 6 months, no significant difference was observed between all the three groups concerning body weight and BMI. These finding are in conformation with a previous study by Ramalho et al., 2017, where the authors have observed that feeding rat with HFD (containing 45% fat) for a total period of 15 weeks didn’t significantly differ in their body weight when compared to the control group.
In the present study, it was observed that the BAX gene was highly expressed in cardiac tissue of the rats fed with high fat diet (HFD). This observation suggests that 6 months of high fat diet (HFD) ingestion lead to activation of cardiac mitochondrial-dependent apoptotic pathway in male Wistar rats. The results obtained from the current study also revealed that there was an up-regulation of BCL2 and down regulation of BAX in rats fed with high fat diet (HFD) supplemented with vitamin D, which indicates to the probable protective effect of vitamin D on the cardiac tissue by mitigating mitochondrial-dependent apoptosis. Our findings are compared with the report of Cheng et al. (2013), which showed induced-cardiomyocyte apoptosis in hamsters fed with high fat diet (2% cholesterol, 1% garlic oil) for 8 weeks with simultaneous increase in the levels of pro-apoptotic proteins BID and BAX, whereas the level of anti-apoptotic protein BCL2 was observed to be decreased. Furthermore, the findings of Zhu et al. (2007) showed elevation in the cardiac expression of BAX along with decreased expression of BCL2 in pigs fed with high fat diet for 12 weeks.
The genetic effects of high fat diet (HFD) intake on BAX expression extended beyond the cardiac tissue to the vascular smooth muscle cells where (Perales S, Alejandre MJ, Palomino-Morales R, Torres C, et al., 2009) in their in vitro study it was observed that addition of 25-hydroxycholesterol to cell culture led to upregulation of BAX expression in the group that received high fat diet (HFD). The cardio protective role of vitamin D in association with the reduction of the elevated levels of Bax and caspase-9 was shown in the study of Wang et al. (2013); the study showed that calcitriol inhibited apoptosis by modulating the proteins that play critical role in the mitochondrial-dependent apoptotic pathway, which matches with the observation of the present study.
Conclusion and Recommendations
The results obtained from the current study confirm the negative influence of high fat diet intake on cardiomyocytes by enhancing myocardial independent pathways of apoptosis in wistar rats. The observations made in the present study extended the understanding of the cardiac beneficial effects of vitamin D supplementation of the high fat diet against chronic consumption of high fat diet (HFD) and thus highlighted an emerging probable protective role of vitamin D supplementation.
Conflict of Interest
The authors declare no conflict of interest.
Acknowledgments
I am deeply indebted to my supervisor Prof. Zienab Alrefaie, Professor in Physiology Department, Faculty of Medicine. King Abdulaziz University, for her guidance during design and planning of the current work. Her constant help, support, patience, valuable recommendations and constructive criticism over all the period of this course of work cannot be rewarded.
I am especially thankful for Prof. Hussam Awad, Professor in Physiology Department, Faculty of Medicine. King Abdulaziz University, for his guidance and professional scientific help. It wouldn’t be possible for me to take this work to completion without his incredible support and encouragement.
Special thanks go to all staff in the animal house, Faculty of Pharmacy, and Genome Center, King Abdulaziz University. This article contains the results and funding of research project that is funded by king abdulaziz city for science and technology (KACST) Grant No.1-18-03-009-0059.
About the Authors
Corresponding Author
Khadeejah Mesaid Al-Solami
Faculty of Medicine, Department of Physiology, King Abdulaziz University, Jeddah, Saudi Arabia
- Email:
- khadeejahalsolami@gmail.com
References
- World Health Organization (2015) "Obesity" http://www.who.int/topics/obesity/en/
- Fitchett D (2015) The metabolic syndrome is an important concept in therapeutic decision-making. Can J Cardiol 31: 596-600. https://doi.org/10.1016/j.cjca.2014.10.037
- Chorin E, Hassidim A, Hartal M, Havakuk O, et al. (2015) Trends in Adolescents Obesity and the Association between BMI and Blood Pressure: A Cross-Sectional Study in 714,922 Healthy Teenagers". Am J Hypertens 28: 1157-1163. https://doi.org/10.1093/ajh/hpv007
- Hubert HB, Feinleib M, McNamara PM, Castelli WP (1983) Obesity as an independent risk factor for cardiovascular disease: A26-year follow-up of participants in the Framingham Study. Circulation 67: 968-977. https://doi.org/10.1161/01.cir.67.5.968
- Swinburn B and Egger G (2002) Preventive strategies against weight gain and obesity. Obes Rev 3: 289-301. https://doi.org/10.1046/j.1467-789X.2002.00082.x
- Kang JH and Kang JY (2015) Lifestyle measures in the management of gastro-esophageal reflux disease: clinical and pathophysiological considerations. Ther Adv Chronic Dis 6: 51-64. https://doi.org/10.1177/2040622315569501
- Dyson J, Jaques B, Chattopadyhay D, Lochan R (2014) Hepatocellular cancer: The impact of obesity, type 2 diabetes, and a multidisciplinary team. JHepatol 60: 110-117. https://doi.org/10.1016/j.jhep.2013.08.011
- Memish ZA, Bcheraoui C, Tuffaha M, Robinson M (2014) Obesity and associated factors--Kingdom of Saudi Arabia. Prev Chronic Dis 11: E174. https://doi.org/10.5888/pcd11.140236
- Earthman CP, Beekman LM, Masodkarand K, Siblay SD (2012) The link between obesity and low circulating 25-(OH) D concentration: consideration and implications". International Journal of Obesity. 36: 387-396. https://doi.org/10.1038/ijo.2011.119
- Assalin HA, Rafacho B, Santos P, Ardisson L (2013) Impact of the length of vitamin D Deficiency on cardiac Remodeling. Circ Heart Fail 6: 809-816. https://doi.org/10.1161/circheartfailure.112.000298
- Ardawi M, Sibiani A, Bakhsh T, Qari M (2012) High prevalence of vitamin Deficiency among healthy Saudi Arabian men: relationship to bone mineral density, parathyroid hormone, bone turnover markers, and lifestyle factors. Osteoporosis Int 23: 675-686. https://doi.org/10.1007/s00198-011-1606-1
- Burgmaier M, Sen S, Philip F (2010) Metabolic adaptation follows contractile dysfunction in the heart of obese Zucker rats fed a high-fat "Western" diet". Obesity (Silver Spring, Md.) 18: 1895-1901. https://doi.org/10.1038/oby.2009.500
- Vieth R (2004) Why the optimal requirement for Vitamin D3 is probably much higher than what is officially recommended for adults. The Journal of Steroid Biochemistry and Molecular Biology 89-90: 575-579. https://doi.org/10.1016/j.jsbmb.2004.03.038
- Ramalho L, Jornada MN da, Antunes L C, Hidalgo MP (2017) Metabolic disturbances due to a high-fat diet in a non-insulin-resistant animal model. Nutrition and Diabetes 7: e245. https://doi.org/10.1038/nutd.2016.47
- Woods SC, Seeley RJ, Rushing PA, D'Alessio D, et al. (2003) A controlled high-fat diet induces an obese syndrome in rats. J Nutr 133: 1081-1087. https://doi.org/10.1093/jn/133.4.1081
- Cheng YC, Chang MH, Tsai CC, Chen TS, et al. (2013) Garlic oil attenuates the cardiac apoptosis in hamster-fed with hypercholesterol diet. Food Chem 136: 1296 -1302. https://doi.org/10.1016/j.foodchem.2012.09.076
- Zhu XY, Daghini E, Rodriguez-Porcel M, Chade AR (2007) Redox-sensitive myocardial remodelling and dysfunction in swine diet-induced experimental hypercholesterolemia. Atherosclerosis 193: 62-69. https://doi.org/10.1016/j.atherosclerosis.2006.08.035
- Perales S, Alejandre MJ, Palomino-Morales R, Torres C, et al. (2009) Effect of oxysterol-induced apoptosis of vascular smooth muscle cells on experimental hypercholesterolemia J Biomed Biotechnol. 1-8. https://doi.org/10.1155/2009/456208
- Wang X, Zhua Y, Wang X, Yang Y (2013) Cardioprotective effect of calcitriol on myocardial injury induced by isoproterenol in rats. Journal of cardiovascular 18: 386-391. https://doi.org/10.1177/1074248413482754
Keywords:
Download:
Full PDF- Share This